Difficulty swallowing (Dysphagia)
- Esophageal stricture: due to long term acid reflux (Gastroesophageal reflux disease), Ingestion of corrosive substance like alkali or acid.
- Severe sore throat (tonsillitis, enlargement of the tonsils).
- Inflammation (eosinophilic esophagitis, radiation esophagitis) or infection (due to candida, herpes simplex) of esophagus
- Tumors: benign or malignant tumor of pharynx or oesophagus.
- Esophageal ring, web or foreign body.
- Masses (enlarged lymph nodes, thyroid gland), tumors or dilated aorta pressing oesophagus from outside.
- Achalasia: Absence of peristalsis (muscle contraction that pushes food) in the oesophagus due to failure of the lower esophageal sphincter (circular muscle) to relax after swallowing.
- Diffuse esophageal spasm.
- Systemic sclerosis (scleroderma): chronic autoimmune connective tissue disease.
- Cranial nerves or spinal cord injury.
- Parkinson’s disease: a chronic, progressive neurodegenerative disorder.
- Stroke.
- Substernal chest pain.
- Weight loss.
- Marked swallowing difficulty.
- Regurgitation and vomiting.
- Significant interference in day to day activities.
- Tonsillitis and epiglottitis are treated with appropriate antibiotics.
- Gastroesophageal reflux disease is treated with proton pump inhibitors (e,g. pantoprazole).
- Mechanical obstruction of oesophagus or throat caused by tumor or foreign body is surgically removed.
- Antibiotic/antifungals for oesophageal infection.
- Nasogastric tube feeding (feeding tube inserted from nose to the stomach) is done to maintain dietary and fluid intake until the causes are identified and resolved.
- Soft and liquid diet which is easy to swallow can be taken to maintain nutritional status of the body and prevent immunity loss.
- Obstructions from enlarged lymph node or external tumors are treated medically or removed surgically.
- Neurologist should be consulted for dysphagia due to diseases of the nervous system.
- Certain devices are also used to dilate or expand the narrow areas of the oesophagus.
- Parkinson’s disease should be treated with Levo-dopa (dopamine).
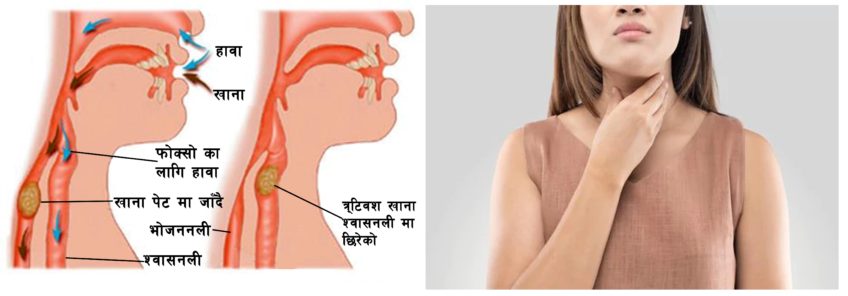
Dysphagia is the inability or difficulty in swallowing food or liquid. Normally, muscles in the throat (pharynx) and esophagus (food pipe) contract rhythmically to move food and liquids from mouth to stomach. Dysphagia occurs when there is a narrowing or lack of coordination of movement (of pharynx or esophagus) due to a local or systemic disease. Dysphagia can cause coughing, choking, drooling, sensation of food getting stuck in throat or chest, weight loss, recurrent aspiration pneumonia or changes in voice or speech. Depending on the location of abnormality, dysphagia can be divided into esophageal dysphagia and oropharyngeal dysphagia. It could be either from an obstruction or from the lack of coordinated movements of oropharyngeal or esophageal muscles.
Common causes:
Obstructions in the throat or oesophagus due to:
Disorders of movement: Loss of normal muscle or nerve function can cause difficulty swallowing, due to:
When to visit the doctor?
Visit emergency department of the hospital if dysphagia is accompanied with breathing difficulty and marked swallowing difficulty and pain.
Seek medical advice and treatment if dysphagia is associated with:
Treatment options
Complete history, physical examination and relevant diagnostic tests are done to find out the cause. Diagnostic tests include barium swallow X-ray of esophagus, upper gastrointestinal endoscopy (EGD), laryngoscopy, oesophageal manometry and pH monitoring of the upper gastrointestinal secretion, chest X ray and CT scan. Following treatment options are considered, depending on the identified cause:



Send us your feedback on this article